Wellness
Faster Healing with Honey
Nature’s Burn Unit

Did you know that you can reduce the time it takes to heal from a minor burn by almost 5 days? It’s true, and we’re going to discuss one of the best ways I’ve found to treat minor burns and abrasions for myself and my family. I’m going to show you how to use honey to heal burns in half the time.
“Out of the eater, something to eat; out of the strong, something sweet.” -Samson: Judges 14:14
My uncle was the first person to show me this simple remedy. He had a collection of honey from all around the world from Iraq to Wyoming. Being the only honey connoisseur I know, I feel fortunate he shared with me such a simple way to care for a common injury. I don’t always trust THE experts, but I do trust MY experts. Before we get to how honey is used to heal burns, I’ll touch briefly on some history and lay out a guideline for knowing if a burn is too severe to treat at home. It is best that you only treat things that you’re capable of safely managing.
Early Writings
The earliest writing I could find that referred to using honey as medicine is from roughly 4000 years ago. There was an ancient tablet found in Nippur, Sumeria (an area about 700+ miles east of the Nile River). It says in part, “grind to a powder, river dust and …(unreadable) then knead it in water and honey and let plain oil and hot cedar oil be spread over it.” This remedy is assumed to have been for some form of injury. However, it is entirely possible that this was also an early recipe for the first gluten free cracker.
Another ancient document referencing honey is known as the ‘Ebers Papyrus’ (1550bc). In this document, honey is mentioned more frequently than any other ingredient for various medicinal concoctions when treating wounds. Honey has apparently been known to have antimicrobial properties for thousands of years. I can almost hear Hippocrates saying: “told ya so,” while Galen’s gladiatorial patients mutter: “muth be nithe”.
3 Levels of Burns
Before we get ahead of ourselves, it’s necessary to circle back around and refresh our memories on the basic types of burns. This is to ensure that we’re clear on what I mean by treating “minor” burns. Severity is determined by both how deep the burn goes, and how much surface area is covered by the burn.
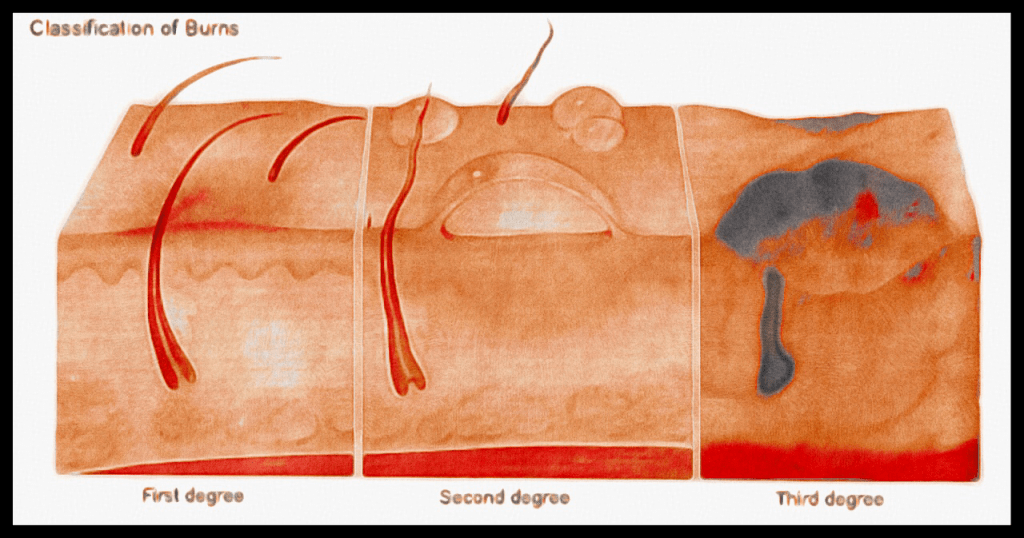
In the diagram (left) and you’ll see the three levels of burn severity. First degree on the left, and third degree (or “full thickness burn”) on the right. If the burn goes through the first two layers and into the hypodermis, it’s considered a full thickness, or a 3rd degree burn.
Partial thickness burns are generally limited to the first and second degree. Once the burn goes through the full thickness of the skin (3rd degree), the chances of serious infection go up. That is why it’s critical to seek trained help for these burns.
3rd degree burns are serious and need to be properly “debrided” or scrubbed. Scrubbing a burn is incredibly painful and should only be done after adequate training. Remember that just because a burn is only partial thickness doesn’t mean it isn’t severe. It is critical to be clear about the amount of area on the body that is burned. So as not to bore you, let’s just assume we’re talking about an area smaller than the size of your palm.
I am not going to address burns located on the groin, near/on the eyes, mouth, or nose. If you or someone you know gets a burn in any of the areas I just mentioned, immediately seek trained medical help.
Note: If a burn goes all the way around a body part (circumferential burn) or covers a significant portion of the body, or if the burn is electrical or chemical in nature, IMMEDIATELY SEEK EMERGENCY MEDICAL HELP.
With that out of the way, we’ll get on to how you can treat those minor burns safely and even reduce the amount of time it takes to heal.
“Let food be thy medicine, and medicine be thy food”
Attributed to Hippocrates (AKA Hippocrates II) c.460-c.370bc
A greek physician during classical greece
Putting Honey To Work
I first used honey on a rug burn years ago at the prompting of my uncle. It worked like a charm. I applied this easy trick on an egg sized area on my forehead. My uncle was gracious enough to supply me a dab of honey and within 2 days the abrasion was fully healed and the scab painlessly fell away on its own. Within 5 days, the pinkness of the new skin was gone entirely. There wasn’t even a hint of scarring. I only applied honey to the wound during the first 2 days. This is considerably fast healing. Studies conducted in certified medical burn units have also tested honey on major burns with promising results. Thanks to honey, doctors now know how to heal burns in half the time.
I don’t always trust THE experts, but I do trust MY experts.
A study in 2008 mentioned in the UK’s NHS website, 1st and 2nd degree burns healed an average of 4.68 days FASTER than the typical burn treatments used at the time. It is noted that there was no increased risk of infection or skin disorders from using quality honey. I always recommend using raw, organic honey.
So how do you apply it?
Nature’s Burn Unit
Step I
I start every medical intervention with washing my hands when possible.
Step II
It’s important to clean the wound you’re treating as well, whether it be a burn or a cut, scrape, or laceration.
Gently wash (avoid using soaps with essential oils just yet, sometimes that can sting quite ferociously). I keep a bottle of betadine wound wash under my bathroom sink and in my medic bag. After washing, dab dry (do not rub) the burn area with a clean, dry cloth.
Step III
Next, simply dip your finger in the honey and gently spread it directly onto the burn.
Step IV
Apply a bandage large enough to cover the affected area. If it’s a bit larger than a bandaid, you can lay any form of clean dry gauze on top of the honey. Next, tape it to the skin. You can also wrap rolled gauze around the area if you know how to properly do this without cutting off circulation. Take extra care to really secure the bandage if you’re treating a child who’ll be rolling around in the grass minutes after you’re done.
Repeat Steps I-IV Daily
I recommend changing the gauze about once a day. You can wash/re-applying honey in the same manner until the burn is fully healed.
Don’t use “honey sauce” packets from KFC. That is NOT real honey. Make us proud and use organic honey. This ancient method is a safe alternative to antibiotic ointments. And as a bonus, you get considerably faster healing times. In a pinch, this is a safe way to keep a wound clean and to help your body heal itself naturally.
Thanks for reading and don’t forget to share this article to your favorite social media platforms. If you have any natural remedies you’d like to share, we’d love to hear about them! You can submit a completed brief step by step article to wellness@beartariatimes.com. For more articles on Wellness click the link here!
Wellness
Beartaria Times Member Shares History and Benefits of Haymaker’s Punch
Today, we saw a post that will be very beneficial in the coming summer heat, especially for those out in the fields!

Whether it’s valuable resources or witty fun, we find great content on our community app every day. Today, we saw a post that will be very beneficial in the coming summer heat, especially for those out in the fields!
Numismaticbear shared a post introducing some of us to Switchel, also known as Haymaker’s Punch!
This sounds like a great beverage to put together!
Thanks for sharing Numismaticbear!

I tried EC for one week, and I’m never going back. Elimination communication allows your baby to relieve themselves outside their diapers and for you to be in tune with their bathroom needs just as you do with knowing when they are hungry.
This can lead to caregivers becoming more in tune with the baby, giving the baby the option of hygiene, cutting down on waste/laundry, and assisting in earlier toilet training. In many countries today, EC is the standard instead of disposable diapers, just without the fancy name.
Do you use the restroom when you wake up or leave to go somewhere? Well, so does baby, and this is the concept of the four easy catches. If it all sounds complicated, just using time and transition to your advantage is a great place to start. The “four easy catches” are offering the baby the potty upon waking up, at diaper changes, signs of effort, and during the transition (getting in and out of something such as the car seat or baby carrier).
For Mothers (or other caregivers) familiar with EC but have yet to try it because it sounds too daunting, I encourage you to try it!
Before my daughter was born, I knew I wanted to use cloth diapers and implement EC. But I wanted to do these things as they came organically and not force myself if it brought more stress than benefit. By three weeks, I was using cloth diapers, and by 6 1/2 weeks, I began EC with her.
In the first week, my baby had only a few poopy diapers. She usually lets me know when she needs to go. Sometimes, I miss it, and sometimes, I put her on the potty, and nothing happens. It is important to remember why you started and not focus on the misses.
While this article wasn’t meant to be a complete study on the subject, I did want to introduce others to the practice or share my positive experience with those aware of EC.
Many resources online cover the subject in depth, I encourage mothers to read around if this is new to you.
I just wanted to share that it works! I took it slow and still utilize diapers, but I am super happy I began to try and implement EC.
Just Crushing
Bees Know Best
Bees are truly a marvelous part of God’s creation and one I draw inspiration from daily as I begin the journey of tending to their homes and lives.

By: Pie Lady Bear
I will often sit and watch them. The importance of their continuous coming and going is apparent even at a distance. Bees are truly a marvelous part of God’s creation and one I draw inspiration from daily as I begin the journey of tending to their homes and lives.
The substances that a hive uses to sustain and thrive are ones that we can also greatly benefit from, and, as the winter weather sets in and lips become chapped, were the illumination behind an impromptu batch of lip balm that you may also find useful!
Beeswax; If you can find it from a local beekeeper, who has taken it from a brace comb that is built in awkward places or melted down frames that are no longer in use, the benefit is the added propolis which is a glue-like material made by the bees from tree resins to seal cracks in their hive and contains exceptional healing properties as well as smelling incredible. My husband, DreadNaught Bear, has been making healing salves with beeswax, pine resin, and sunflower oil long before I began keeping bees. You can find his recipe in the second issue of the Beartaria Times Magazine to cure all that ails you! Beeswax can also be found at a local health food store or taken from pure beeswax candles.
Coconut oil; I prefer organic and use it in my cooking as well, so it’s worth buying a jar.
Peppermint oil; I only added three drops for the small glass jar of lip balm as using more would cause a slight burning sensation and takes away from the amazing smell of the beeswax.

I made my lip balm in a small jar that is placed in a pot on the stove with about an inch of water surrounding it and a covered lid. Turn on low heat and frequently check until the wax and coconut oil have melted, then add the few drops of peppermint oil, stir and allow to cool. That’s it! So simple, and depending on the amount you would like to make or the size of your container, I went with a ratio of 2:1 coconut oil to wax, and that made for a smoother consistency. God Bless the Bears as we strive to focus our lives around the good, the true, and the beautiful 🤎
Onward!
-

 Just Crushing2 weeks ago
Just Crushing2 weeks agoChristopher Gardner Completes First Dome Framing Project in Missouri: Exclusive Interview
-

 Just Crushing2 months ago
Just Crushing2 months agoBeartaria Ozark Campground Launches Community Forum!
-

 Just Crushing2 months ago
Just Crushing2 months agoMap it! – Discover Beartarians Living, Working, and Crushing Near You!
-

 Just Crushing2 months ago
Just Crushing2 months agoWhy Do We Feel So Free?
-

 Lifestyle2 months ago
Lifestyle2 months agoReconnect and Rejoice: Beartaria Times Weekly Challenge
-

 Reports2 months ago
Reports2 months agoReport: EF-1 Tornado Touches Down In The Ozarks
-

 Business2 months ago
Business2 months ago3000 Members In Our Business Group!: This Week On Our Community App!
-

 Wellness2 months ago
Wellness2 months agoBeartaria Times Member Shares History and Benefits of Haymaker’s Punch